Allergic conjunctivitis is one of the most common diagnoses made in the OPD of an ophthalmologist these days. Most of these patients are children or young adults. Much of this increasing incidence of allergy can be attributed to environmental pollutants, exposure to dust, smoke, pollen, animal hair, and mold. These substances are widely present in our surroundings, especially in the spring and summer seasons. Many children have a history of other allergies like dermatitis, asthma, and allergic rhinitis as well. Certain individuals like those working in laboratories, sitting in air-conditioned rooms, passively inhaling the smoke ( even from agarbatties and mosquito repellants ) are at higher risk of allergic conjunctivitis. Long time contact lens wearers are also at increased risk.
Symptoms of Allergic conjunctivitis
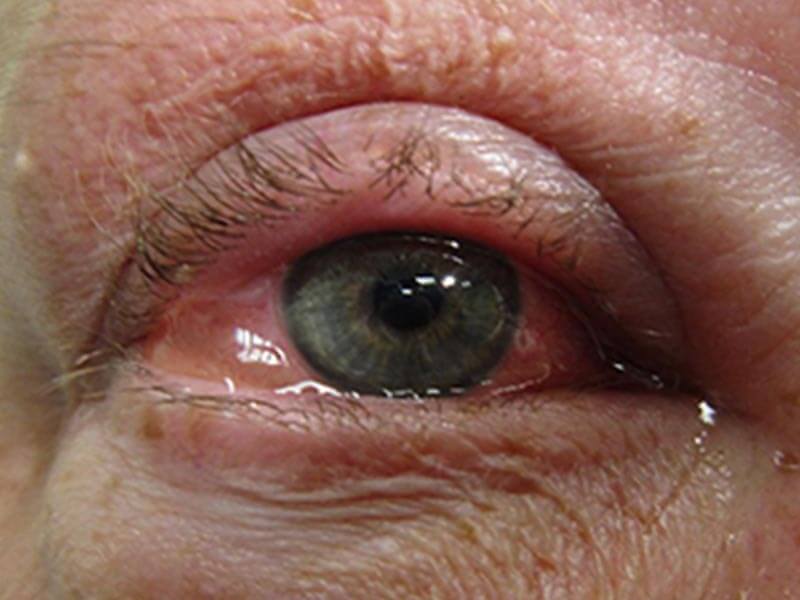
The most common symptom of allergic conjunctivitis is the intense itching of the eyes accompanied by redness, watering, ropy discharge, pain, and occasional blurring of vision. Many afflicted individuals have a habit of touching their eyes and pulling out strands of mucus. Some children with chronic eye rubbing develop dark circles around their eyes and a muddy colour of the conjunctiva. Eye symptoms may be accompanied by sneezing, running nose, and wheezing
Allergic conjunctivitis may be seasonal or perennial. Early spring and summer may herald the onset of these symptoms. Usually, the symptoms may resolve with medication and reappear later on exposure to allergens
Lifestyle and environmental modifications are the first lines of prevention of allergies. A detailed history is mandatory to elicit the cause of allergy and aggravating factors. Parents must be advised to keep the child away from dust, smoke, animal hair, and pollen. Eye rubbing should be strictly discouraged. Vacuum cleaning and wet mopping of floors are useful. Cold compresses and lubricating drops should be used frequently to give comfort to the eyes and dilute the concentration of inflammatory substances in the conjunctiva
In more severe cases, antihistaminic and mast cell stabilizing eye drops and tablets may be used. Sometimes steroid eye drops are advised but they should be used with caution as many side effects are associated with their long term use
Vernal keratoconjunctivitis is a serious form of allergic conjunctivitis which if not treated can have vision-threatening complications. Sometimes it is associated with keratoconus which is a progressive ectasia of the cornea along with thinning and irregular astigmatism
To summarize, allergic eye disease occurs commonly in our country. It can be easily diagnosed and treated by adopting environmental modifications and using eye drops. Always use eye drops after consulting your eye specialist. Early intervention can prevent vision-threatening complications of severe allergic conjunctivitis
Also Read– All About Cataract | Symptoms, Doctors, Treatments